Osteoporosis affects an estimated 10 million people in the United States aged 50 and up. The majority of these people are women, with only around 2 million men among them.
Osteoporosis affects an estimated 10 million people in the United States aged 50 and up. The majority of these people are women, with only around 2 million men among them. Amid startling prevalence, various organizations’ guidelines have suggested osteoporosis screening in women and men starting at a certain age or based on certain risk factors for years.
For example, the US Preventive Services Task Force (USPSTF) issued guidelines that urge universal osteoporosis screening for women 65 and older and targeted screening for those younger than 65 with risk factors for osteoporosis. Unfortunately, despite efforts to increase the use of osteoporosis screening, recent studies back up what has long been known: Even in women who have had a first hip fracture, utilization remains unacceptably low.
This article will look into the importance of osteoporosis screening and several recommendations from experts.
What Is Osteoporosis?
Osteoporosis is a bone disease wherein the levels of a person’s bone density and mass decrease. In other words, it is when bones become brittle or weak due to various reasons: aging (menopausal stage for women over 65 years old), chain-smoking, insufficient calcium intake, estrogen deficiency, inadequate vitamin D, and low body weight. It may sound natural to have a lesser bone density as one grows older but what makes osteoporosis distinct is the permanent pain that a person will experience every day. In addition, some may lose height and have stooped or hunched posture when the disease affects the bone of the spine.
There are various factors and recommendations before conducting an osteoporosis screening test, like who is qualified? Why is there a need to do the test? What are the screening test recommendations that are convenient and safe for the patient? These things need to be addressed beforehand.
Who Needs To Undergo Osteoporosis Screening?
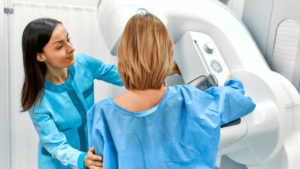
Women over 65 years old, menopausal women under 65 years old with similar risks to the first one, and men over 70 years old are the usual patients who undergo osteoporosis screening tests. As can be observed from the enumerations, women are the ones who usually undergo the said tests because they are more prone to having osteoporosis. This bone disease stops estrogen production, leading to scarcity of the same needed for stronger bones.
Women 65 Years Old Or Older With No History Of Fractures
It is natural for women over 65 years old to decrease bone density or bone mass, so even though they don’t have a history of fractures, it is still recommended to undergo screening tests. By doing this, they will be able to prevent further bone damages.
Women Younger Than 65 Years Old With Fracture Risk
A risk assessment test will check one’s bone density if she is prone to Osteoporosis in 10 years. If women were assessed to have future fractures or bone diseases, they are encouraged to undergo bone mass density tests.
Men With No Prior Bone Fractures
It is for men over 70 years old that are worried about their bones getting weak. Yet, according to a study, men are not recommended to undergo osteoporosis screening tests. The reason behind this is a lack of evidence in the necessity of doing so.
Why Is There A Need For Osteoporosis Screening?
Osteoporosis screening is not recommended to everyone. Medical practitioners cannot put someone through tests unless they qualify to be tested (age is above 65 years old for women and 70- years old for men). However, there are also benefits of early osteoporosis screening for qualified persons, like fracture prevention.
To ensure that patients will not experience any more complications in the future, especially in their bones, having a preventive check-up will help a lot. Bone fractures, especially in the hips and lumbar spine, are severe effects of disregarding the mandate of doctors to undergo osteoporosis screening. Screening tests will help figure out how their case will be treated carefully.
Aside from this, ensuring that they get treated right away once the results come out will help their bodies maintain and improve their mobility.
No studies or evidence will state the harms of early osteoporosis detection and screening in terms of side effects.
Screening Test Recommendations
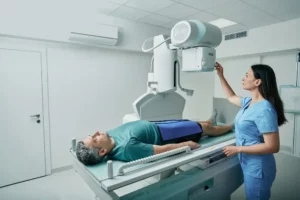
There are various methods to screen persons with osteoporosis, like Dual-Energy Absorptiometry (DXA), Quantitative Ultrasound, and Bone Density Test.
Dual-Energy Absorptiometry (DXA)
There are two (2) kinds of DXA, namely, Central DXA and Peripheral DXA. In the former, the measurement will be done in the hip and lumbar spine. While in Peripheral DXA, the usual bones tested or measured are the lower forearm and heel. Both of these tests use radiation similar to X-ray to get a person’s Bone Mass Density data.
Quantitative Ultrasound
Unlike the first one, Quantitative Ultrasound uses ultrasound not to measure but only to evaluate the patient’s peripheral bone sites like the calcaneus. The difference between this method and DXA is that the tool can be used not just in a single location. In other words, QU will be able to measure the density of different bones in the body. Thus, the medical practitioner will have the opportunity to check various areas in one session.
Bone Density Test
Last but not least, doctors may also have bone density test recommendations for patients who qualify for such a screening method. Similar to DXA, a bone density test uses an X-ray to measure bone mass. What makes this one distinct is its capability to evaluate patients’ bones and predict their bone fracture risks. For example, suppose the evaluation states that one has a chance of osteoporosis or has weak bone mass density; doctors can recommend treatment/medications to ensure that they will not experience permanent pain in their bones in the future.